Spectral characteristics of the internal jugular vein and central venous pressure pulses: a proof of concept study
HTML: 106
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Authors
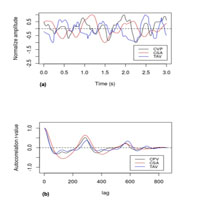
In this proof-of-concept study the impact of central venous pressure (CVP) on internal jugular veins cross-sectional area (CSA) and blood flow time-average velocity (TAV) was evaluated in eight subjects, with the aim of understanding the drivers of the jugular venous pulse. CVP was measured using a central venous catheter while CSA variation and TAV along a cardiac cycle were acquired using ultrasound. Analysis of CVP, CSA and TAV time-series signals revealed TAV and CSA to lag behind CVP by on average 0.129 s and 0.138 s, with an inverse correlation between CSA and TAV (r= –0.316). The respective autocorrelation signals were strongly correlated (mean r=0.729-0.764), with mean CSA periodicity being 1.062 Hz. Fourier analysis revealed the frequency spectrums of CVP, TAV and CSA signals to be dominated by frequencies at approximately 1 and 2 Hz, with those >1 Hz greatly attenuated in the CSA signal. Because the autocorrelograms and periodograms of the respective signals were aligned and dominated by the same underlying frequencies, this suggested that they are more easily interpreted in the frequency domain rather than the time domain.
How to Cite
PAGEPress has chosen to apply the Creative Commons Attribution NonCommercial 4.0 International License (CC BY-NC 4.0) to all manuscripts to be published.

 https://doi.org/10.4081/vl.2021.9732
https://doi.org/10.4081/vl.2021.9732





